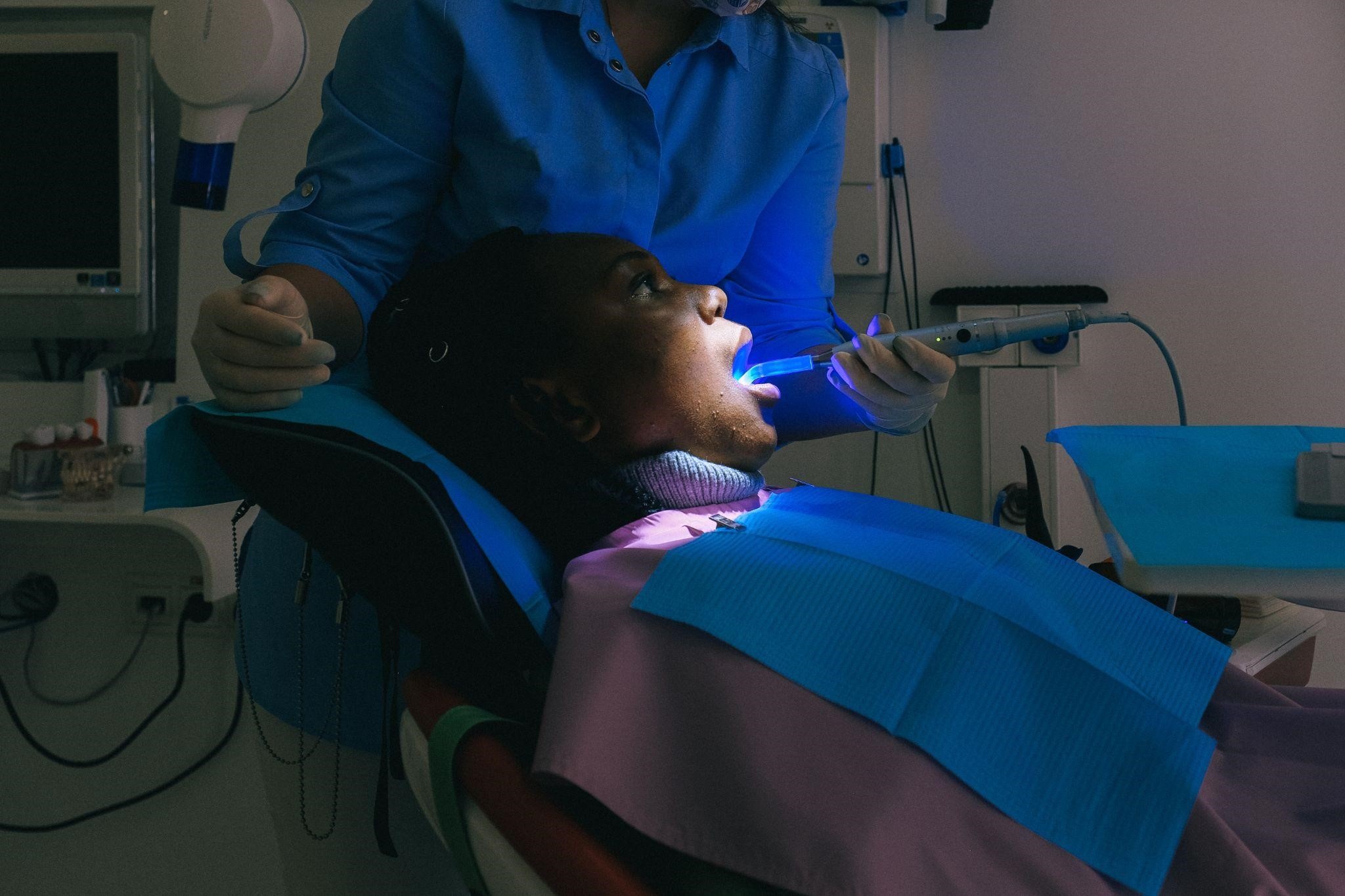
Dental Care Tips for diabetics
Dental Care Tips For Diabetics People is one of the most essential things to care about. A person with diabetes is more prone to get problems with teeth.
Diabetes is a major health issue that has been affecting more people than we know. In the United States alone, 29 million citizens have diabetes and about 1 out of 10 don’t even realize they’ve got it!
This makes it hard for them to manage their condition which can lead not only to poor management but also to complications over time such as kidney failure if left untreated or improperly controlled with medications like insulin shots at night when you go into type 2 DM2 – do NOT let this happen!
The good news? There’s hope through lifestyle changes including eating healthier foods high on fiber content–and cutting back.

Why are people with diabetes more likely to develop oral health problems?
There are many reasons why people with diabetes may experience oral health problems. One of the major ones is because blood sugar levels can get out of control, leading to weakened white cells in your mouth that fight off bacterial infection.
This makes it more likely for you to develop gum disease or other dental issues (such as cavities), especially since studies have found controlling these disorders lowers the risk of organs being damaged by diabetes itself!
Why does anemic cell function matter when talking about preventing Oral Health Problem-related disabilities? The answer has everything doodle inside – from the genetic background all through diet choices made today. Check the below following tips
1. Brush twice a day, after each meal if possible.
Brushing cleans teeth by removing plaque and food debris from the surface of the tooth enamel. Plaque is a bacterial film that constantly forms on the surfaces of our teeth as we eat and drink. If left in place, plaque can harden into tartar which causes gingivitis (inflammation of the gum tissue) and periodontal disease (gum disease). Plaque also harbors numerous types of pathogenic bacteria which may cause oral infections such as abscesses or cellulitis.
2. Floss once a day.
Flossing cleans between teeth that are tightly packed together like the ones you find in your back molars, where toothbrush bristles cannot reach. It is important to floss daily because it can dislodge food particles and plaque that accumulate between these tight spaces causing cavities and gum disease.
3. Take Oral Probiotics
Take an oral care probiotic supplement like OraWellness Dental Defense. Oral care probiotics help balance levels of pathogenic (bad) bacteria vs. beneficial (good) bacteria in the mouth, promoting overall dental health.
4. Replace your toothbrush every 3-4 months
You can Replace your toothbrush every 3-4 months or sooner if the bristles become frayed or worn out as they may be too harsh on the gums.
You should also replace your toothbrush after you’ve had a cold, since the bristles can harbor bacteria that may reinfect your mouth.
5. Drink fluoridated water
Drink fluoridated water is to reduce the risk of cavities and other dental problems . Fluoride helps strengthen tooth enamel against acid wear from food and drinks that cause tooth decay.
6. Reduce Plaque accumulation on teeth
Reduce snacking between meals to lessen plaque accumulation on teeth. Snacking stimulates bacterial activity which adds to acids being produced around teeth causing enamel loss through erosion.
7. Schedule a Visit with your dentist
Schedule an annual visit with your dentist for professional cleaning. Your dentist will remove tartar buildup using special instruments so as not to irritate or damage sensitive gum tissue.
Visit your dentist right away if you have any dental problems like unexplained pain, swelling, or bleeding gums.
Dentists can perform restorative work to treat damage to teeth and gum tissue caused by chronic disease/inflammation such as gingivitis and periodontal disease.
Diabetics are more likely than other people to develop these types of problems because they have an elevated risk for developing various medical conditions that affect the immune system including gum disease, necessitating early intervention with professional treatment. Gum health is just as critical as oral hygiene – if not more so – because it may contribute to systemic (whole body) health concerns.
Always consult a qualified healthcare provider before changing your diet or using any supplements.
FAQ’s
What is the recommended blood glucose level for tooth removal?
Answer: A level of 105-110.
It is recommended to have a level of 105 or 110 for your blood glucose before the procedure. Checking the sugar in your blood will tell you how much insulin you will require before and after the surgery. The more glucose, the more likely it is that inflammation will set in, causing damage to healing tissue. This can prolong recovery time from ten days to three weeks instead of two weeks if one has a lower sugar level before surgery.
Is chewing gum bad for diabetics?
It all depends on how often you chew it and for how long, but in general it’s not something that should be eaten for lunch or dinner. Chewing gum produces glucose intermittently, but the action of chewing (and especially motion about one’s lower jaw) stimulates saliva production – which is typically high in sugar. So you’re better off without the gum if you can help it.
Good post about diabetes really informative. check this site to also provide premium care for dental health.
Good information about dental care tips for diabetics.